Biomechanics: measuring the human body

Research with heart and mind – and mathematics
How exactly cardiovascular tissues such as blood vessels or the heart muscle change in the course of a lifetime, during disease and after an operation, differs from person to person. Much is still unknown. And this is where the relatively recent science of biomechanics comes in – as an interface between medicine and technology. Researchers at TU Graz’s Institute of Biomechanics are using engineering methods of calculation to describe human “pipes” and “pumps”. To characterise the material properties of soft biological tissue and thus to detect or predict changes, for example in blood vessels and heart tissues, samples of healthy and diseased tissues are measured in test devices which have been developed at the Institute. The results serve as a basis for computer-aided modelling by which tissue changes can be graphically represented.
Treatment is becoming more personalised
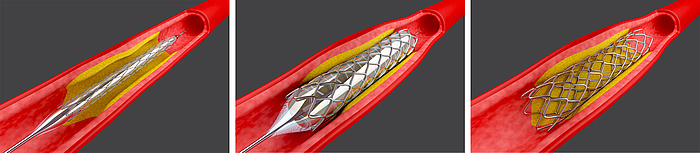
How exactly can the findings obtained at the Institute of Biomechanics help in practice? One example is the more effective and individual treatment for aortic dissection than was previously the case. This disease is characterised by a tear in the inner wall of the vessel. Blood flows into the next layer of the aorta and forms a bulge which changes the blood flow in the aorta. Various areas are no longer sufficiently supplied with oxygen, thus possibly leading to a stroke or acute kidney failure, among other things.In the surgical treatment of an aortic dissection, either a part of the aorta is replaced or a stent implanted – a small, supportive mesh-like tube which keeps the vessel open. Both approaches bear considerable risks, and determining the optimum method or the best time for a surgical intervention always represents a challenge.
This research topic is anchored in the Field of Expertise “<link https: www.tugraz.at en research forschungsschwerpunkte-5-fields-of-expertise human-biotechnology overview-human-biotechnology _blank int-link-external external link in new>Human & Biotechnology”, one of the five strategic research foci at TU Graz.
Kontakt
Phone: +43 316 873 35500
<link int-link-mail window for sending>holzapfel@tugraz.at
Gerhard SOMMER, Dipl.-Ing. Dr.techn.
Phone: +43 316 873 35505
<link int-link-mail window for sending>sommer@tugraz.at Institute of Biomechanics
Stremayrgasse 16/2
8010 Graz, Austria
<link http: www.biomech.tugraz.at _blank int-link-external external link in new>www.biomech.tugraz.at



